





 Order Treatment Online
Order Treatment Online
 Diseases and Conditions
Diseases and Conditions
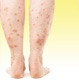
Lichen planus is a recurrent rash that is due to inflammation. The rash is characterized by small, flat-topped, many-sided (polygonal) bumps that can grow together into rough, scaly patches on the skin. There may also be a rash in the lining (mucous membranes) of the mouth or vagina.
Lichen planus is a very curious skin condition, the effects of which are localized to the areas of involvement. (Lichen refers to a tree moss while planus is Latin for flat = like a flat tree moss.)
The major point of distinction of lichen planus from eczema, psoriasis, and other common rashes is its color -- lilac or violet. The textbooks call it "violaceous."
Lichen planus itches with an intensity that varies in different people from mild to severe.
The onset of lichen planus can be sudden or gradual. The first attack may last for weeks or months, and recurrences may happen for years. Children are not often affected by lichen planus. The bumps at first are 2 to 4 mm in diameter, with angular borders, and a violaceous color. At the onset of the disease, new bumps may appear at sites of minor skin injury, such as a superficial scratch. An excess of pigment (hyperpigmentation) may develop in the affected skin as the lesions persist. Rarely, a patchy scarring balding (alopecia) of the scalp occurs.
The appearance of lichen planus depends on whether the skin or the lining (mucous membranes) inside the mouth or vagina are affected:
More troublesome, although rare, is erosive lichen planus, which can be quite sore and uncomfortable. This erosive form typically causes the patient to complain of the shallow and often quite painful, recurrent ulcers in the mouth.
Lichen planus can affect the female genitals, including the vagina. This condition can be confused with sexually transmitted diseases (STDs), although lichen planus is neither sexually transmitted nor contagious.
Sometimes, lichen planus produces pits and grooves in the nails as well.
Next: How is lichen planus diagnosed?
Usually, lichen planus is relatively straightforward to diagnose. Physicians can make the diagnosis in typical cases simply by looking at the rash. If necessary, a skin biopsy may be done to help confirm the diagnosis. Under the microscope, lichen planus is distinctive in appearance.
This tell-tale appearance under the microscope can be valuable in ensuring that the rash or spots are lichen planus. Persistent oral or vaginal lichen planus, with spots that thicken and grow together, can sometimes be difficult to distinguish clinically from whitish precancerous plaques called leukoplakia. A biopsy can be helpful in this situation.
Widespread lichen planus with erosions in the mouth can also be confusing. A biopsy may be required to distinguish this from other conditions such as candidiasis (yeast infection), carcinoma (cancer), and ulcers in the mouth (aphthous ulcers).
In most cases, the cause of lichen planus is unknown.
Some drugs, such as those containing arsenic, bismuth, or gold can cause a reaction that is indistinguishable from the rash of lichen planus. Exposure to certain chemicals used in the development of color photographs can also produce a similar rash. The long-term use of the drugs quinacrine or quinidine (used for malaria, certain microscopic organisms, and worms) may produce hypertrophic lichen planus of the lower legs and other skin and body- wide (systemic) disturbances. Other unusual causes of lichen planus include liver disease and what is called graft-versus-host disease in people who have received a transplant.
Most cases of lichen planus are relatively mild. Affected individuals who do not have symptoms do not need treatment.
If the itch or appearance of the rash is unpleasant, topical corticosteroid creams may be of help. Topical steroid creams that, for example, are under wrapping or taped at bedtime may also be useful. For localized, itchy, thick lesions, injections of corticosteroids may be given. Antihistamines may blunt the itch, particularly if it is only moderate. This effect is in part due to the sedative effect of antihistamines.
In more severe cases, physicians may recommend oral medications or therapy with ultraviolet light. Orally taken medications may include a course of oral corticosteroids such as prednisone. However, the itching may return after the drug has been discontinued. A low-dose oral corticosteroid every other morning may be also prescribed. With continued itching, ultraviolet light (PUVA) treatment may help. For painful lesions within the mouth, the use of special mouthwashes containing a painkiller (such as lidocaine) before meals may provide some relief. Any drug or chemical suspected of being the cause of the lichen planus should of course also be halted.
Lichen planus usually goes away by itself in time. Some drugs can produce rashes that are similar in appearance to lichen planus. These rashes can be distinguished from lichen planus in that they go away when the offending drug is stopped.
Lichen planus, by contrast, usually persists quite a while before resolving. The average duration of the condition is 4 years. Even after going away, lichen planus may recur. The disease is thus paradoxical in that it tends to be self-limiting but may recur after years. It is usually not associated with any body-wide (systemic) diseases or problems.